Anencephaly
- mrsaepts
- May 30, 2023
- 5 min read
BY Pitchapa Srisamut
EDITED BY Pakpol Kunopasvorakul
What is Anencephaly?
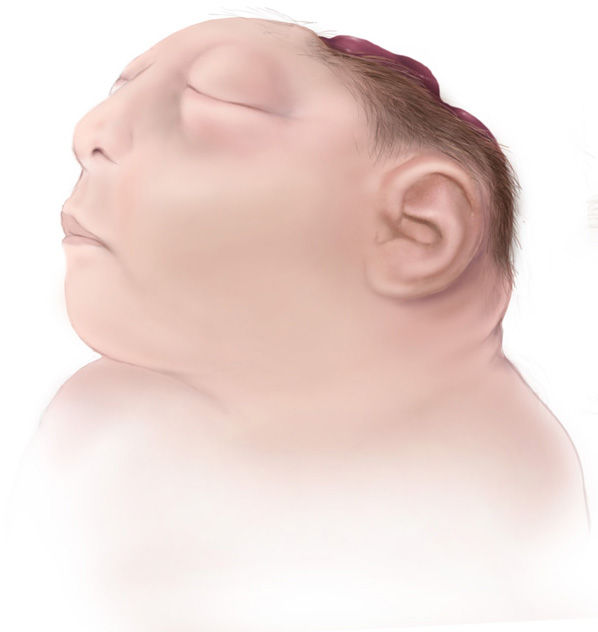
Anencephaly (a-nuhn-seh-fuh-lee) is a kind of neural tube defect (NTD) where a baby is born with the absence of major portions of the brain and skull. During the third and fourth weeks of pregnancy, the neural tube forms and closes in order to help form the embryo’s brain (upper end of the tube), skull, spinal cord, and backbone (lower end of the tube). However, in an infant with anencephaly, the upper end of the neural tube fails to close entirely; therefore, resulting in missing parts of the brain such as the forebrain and oftentimes, the cerebrum as well. While there are some remaining parts of the brain, they are usually not covered by any bones or skin.
Even though anencephaly is a serious neurological disorder, it is rather rare. According to an article by Cleveland Clinic, around one out of 5,000 to 10,000 infants is born with anencephaly and female babies have higher chances of being affected by this condition than males (Anencephaly: Neural Tube Defect, Birth Defect, Causes, Prevention, n.d.). Moreover, these pregnancies with anencephaly commonly end in miscarriage or stillbirth. Hence the little prevalence in newborns.
Causes, Risk Factors and Symptoms
Causes & Risk Factors
Despite the fact that the causes among most infants with anencephaly are unknown, studies have indicated that the condition can be caused by a combination of several factors. Genetics, environment, and nutrition play a crucial role in the development of anencephaly during pregnancy.
The infant’s own genes or chromosomes along with other genetic disorders may affect the likelihood of developing anencephaly. Regardless of how genetics may be able to influence the chances of anencephaly development, it is reported that on regular circumstances, the condition does not demonstrate a clear pattern of inheritance, for the majority of anencephaly cases have occurred sporadically. In other words, patients affected by anencephaly do not need to have a family history of the condition. However, based on an article by MedlinePlus provided by the National Library of Medicine, babies born to parents who have had an anencephalic child before have an increased risk of developing the condition when compared to the general population (Anencephaly: MedlinePlus Genetics, n.d.).
The mother’s contact with the environment has an impact on the baby’s risk; take temperature as an example. If, at the period where the baby’s neural tube is supposed to be closing, the mother had come in contact with high temperature—for instance, entering a sauna, using a hot tub, or having a fever—this may increase the risk of anencephaly development.
Nutritional factors revolve around the mother’s health, nutrients intake, medication, and/or drug use. These include folic acid (vitamin B9) deficiency, uncontrolled diabetes, obesity, opioid (codeine, oxycodone, morphine, etc.), and the use of medications used to treat seizures, bipolar disorder and migraines (phenytoin, carbamazepine, valproic acid, etc.). Such factors, as stated, may be one reason among many others to cause rise in the risks of anencephaly development.
Symptoms
There are a number of methods to detect signs of anencephaly during pregnancy. However, most symptoms are present at birth. Based on the information provided by Boston Children’s Hospital, there are three common symptoms: missing bony covering on the back of the head, absence of bones on the front and the sides of the head, and folding of ears (Anencephaly | Boston Children’s Hospital, n.d.). Other symptoms of anencephaly, which can result in further birth defects include cleft palate (a condition where the roof of a child’s mouth does not close entirely) and congenital heart defects.
Diagnosis
Diagnosing anencephaly can be done during pregnancy or done physically after the baby is born. Sometimes anencephaly is not diagnosed until the birth of the baby. On the other hand, doctors may conduct tests for neural tube defects as part of the mother’s prenatal care in order to diagnose anencephaly early on. Examples of these diagnostic tests are described as follows:
Ultrasound
Ultrasound, as the name suggests, uses high-frequency sound waves to generate images of the baby inside the mother’s womb. From these images, doctors are able to have a look and search for any abnormalities in the brain, skull, and spine.
Fetal Magnetic Resonance Imaging (MRI)
Similar to ultrasound, MRI is a technology used to create pictures of the inside of a human body. The difference is that an MRI would use high-powered magnets to create a more detailed image of a baby’s tissues and bones, rather than using high-frequency sound waves. Doctors use the image generated by MRI to check the baby’s spine and brain in detail.
Quad Marker Screening
Quad Marker Screening is a test done during the second trimester to look for these four factors in blood: alpha-fetoprotein (AFP), unconjugated estriol (UE), human chorionic gonadotropin (hCG), and inhibin-A. Abnormal levels of these factors may indicate high chances of neural tube defects as well as other genetic disorders. AFP is produced by the baby's liver and a high level of it could indicate higher risks of anencephaly and other neural tube defects, for instance, spina bifida. Additionally, this could also indicate twins or that the stage of pregnancy is further in than expected. Whilst low levels of AFP may be a sign of having a child with Down Syndrome.
If the levels of the protein inhibin-A and the hormone hCG are higher than normal, this could be a sign indicating an increased risk of Down Syndrome. As for the hormone UE, low level of it could mean a larger risk of the baby's Down Syndrome development.
Amniocentesis
Amniocentesis is a test where doctors will withdraw amniotic fluid from the amniotic sac in order to check for AFP and an enzyme called acetylcholinesterase. High levels of AFP or acetylcholinesterase may indicate that the fetus has a neural tube defect.
Prevention & Treatment
Prevention
Preventing anencephaly is not always possible. Still, the infant’s chances of developing anencephaly can be reduced by multiple ways. These include:
Even though one may not plan to become pregnant in the near future, taking enough folic acid daily (400 micrograms) is still recommended.
Avoid certain medications used to treat seizures, migraines, and bipolar disorder. Using opioids during pregnancy should also be avoided.
Refrain from entering saunas and using hot tubs to keep the body temperature at a normal level. In case of a fever, one should have a discussion about reducing fever with their doctor first.
Maintain a healthy weight and conditions. Consulting a doctor if one has obesity or diabetes may be helpful for managing one’s health during pregnancy and keeping the baby in safe conditions.
Treatment
Unfortunately, scientists and researchers have not yet found a treatment for anencephaly as well as other neural tube defects. As previously mentioned, most pregnancies with neural tube defects result in miscarriages or stillbirths. Those infants who were not miscarried or stillborn pass away after a few hours or days. Although it is not possible to cure or save a baby from anencephaly, doctors could help families to make the most out of the time they and their babies have together.
Reference:
Anencephaly. (n.d.). National Institute of Neurological Disorders and Stroke. https://www.ninds.nih.gov/health-information/disorders/anencephaly
Anencephaly: Neural Tube Defect, Birth Defect, Causes, Prevention. (n.d.). Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/15032-anencephaly
What is Anencephaly? (2021, June 17). WebMD. https://www.webmd.com/baby/what-is-anencephaly
Anencephaly | Boston Children’s Hospital. (n.d.). https://www.childrenshospital.org/conditions/anencephaly
Facts about Anencephaly | CDC. (2020, December 28). Centers for Disease Control and Prevention. https://www.cdc.gov/ncbddd/birthdefects/anencephaly.html
Anencephaly: MedlinePlus Genetics. (n.d.). https://medlineplus.gov/genetics/condition/anencephaly/#inheritance
Professional, C. C. M. (n.d.). Pregnancy: Quad Marker Screen. Cleveland Clinic. https://my.clevelandclinic.org/health/diagnostics/4698-pregnancy-quad-marker-screen
Comments