Obsessive - Compulsive Disorder (OCD) — What is it?
- mrsaepts
- Nov 26, 2022
- 7 min read
Updated: Nov 29, 2022
BY Nannapat Jeamanukoolkit, Siramon Kanchanachittakorn, Nareutadhorn Toasaksiri
Nipitphon Tungkarak, Worathas Wongsatidporn
What is OCD?
Do you have OCD if you always have an urge to wash your hands? The answer is it depends. The information provided in this article would, hopefully, answer what it is and what it depends on.
Obsessive-Compulsive Disorder, or OCD for short, is a mental disorder characterized by recurring, or obsessive, thoughts and urges to do something repeatedly (compulsions).
Approximately 1 - 3% of the population is diagnosed with this disorder. Anyone could be diagnosed with OCD, though the prevalence differs greatly across different demographics. OCD is most prevalent in older teens or young adults. Though onset may begin as early as preschool age up until age 40. Male children are more likely to have OCD than female children, while the tendency is flipped in adults. The weighted cumulative OCD prevalence rates were 5.3% for females and 1.7% for males.
“It’s not about being tidy, it’s about having no control over your negative thoughts. It’s about being afraid not doing things a certain way will cause harm” (What is OCD? - Mind).
Signs and Symptoms
Obsessive-Compulsive Disorder (OCD), as the name suggests, is characterized by the symptoms of both obsessive thoughts and compulsive behavior.
Here’s the United Kingdom National Health Service’s definition:
An obsession is an unwanted and unpleasant thought, image, or urge that repeatedly enters your mind, causing feelings of anxiety, disgust, or unease.
A compulsion is a repetitive behavior or mental act that you feel you need to do to temporarily relieve the unpleasant feelings brought on by the obsessive thought.
Though, you might ask, what does this really mean? The catch is that these thoughts have to be disruptive to daily life – hence its namesake disorder. For people with OCD, these thoughts are abnormally persistent ie. not performing the behaviors commonly causes great distress. People with OCD experience the presence of obsessions and/or compulsions that last more than one hour a day.
Common Obsessive thoughts include:
Fear of getting contaminated by other people or the environment
Disturbing sexual thoughts or images
Fear of blurting out curse words or insults
Extreme concern with order, symmetry, or precision
Fear of losing or discarding something important
Common Compulsive behaviors include:
Repeated actions such as cleaning of household objects; checking locks, switches, or appliances
Excessive or ritualized hand washing, showering, or brushing teeth
Ordering or arranging things in a particular way
Constantly seeking approval or reassurance
Causes and Risk Factors
Genetic Factors – Highest Weight
Genetic factors were proven to also contribute considerably, or the most, to OCD. This disorder tends to run in families; having a relative with OCD increases the risk of having OCD.
Brain and Hormones Mechanism
People with OCD have abnormalities in the orbitofrontal cortex and caudate nuclei. Abnormalities in one or more neurotransmitters such as serotonin, glutamate, GABA, and dopamine were also found to be associated with OCD symptoms.
Presence of Other Mental Comorbidities
OCD is often present in people who have other mental health illnesses. This can include :
Autoimmune disease
PANDAS (Pediatric Autoimmune Neuropsychiatric Disorders associated with Streptococcal Infections) is an illness in children. It causes OCD and/or a tic disorder. This type of OCD could be made worse with a strep throat.
Stress
Stress can trigger obsessive-compulsive disorder onset. obsessive-compulsive disorder is often linked to major life changes, such as the loss of a loved one, divorce, relationship issues, problems in school, or abuse.
OCD left without immediate treatments will grow to be a more severe chronic mental disorder, particularly when the individual is faced with stressful situations. Individuals with obsessive-compulsive disorder will experience any forms of exceeding thinking and behaviors as a form of his or her anxiety or fear that later on affecting the everyday life function
Pregnancy and Postpartum Period
Hormones can trigger symptoms. OCD symptoms may worsen with pregnancy; symptoms can include intense worry over the baby’s well-being.
OCD symptoms are more frequently seen in pregnant women. up to 25% of pregnant women have OCD symptoms. And up to 63.5% in postpartum women. Of note is that most new parents experience intrusive thoughts about their infant, although these thoughts do not necessarily indicate OCD.
Studies describing the relationship between the onset of OCD and gestational time suggest that OCD occurs mostly during the second or the third trimester. Finally, one study noted that there were no significant differences between pregnant women with and without OCD with regard to demographic characteristics, number of gestations and live births, gestational week, having had an abortion, and other gestational complications that my exist. (https://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.681.2122&rep=rep1&type=pdf) A positive family history of OCD was significantly higher in pregnant women with OCD to those compared to without OCD. However, the sample of this study mostly comprised women who had OCD before their gestation.
Impacts
Individuals with OCD struggle immensely to maintain relationships. Apart from obsessive thoughts and compulsive behaviors disrupting normal interaction, the lack of insight into the disorder’s nature amongst the general population could lead to perceptions of unpredictability, pushing away people
According to the WHO, OCD is the 6th largest contributor to non-fatal health loss globally and appears in the top 10 causes of YLD (years lost to disability) in all WHO regions. With that being said, it is no surprise life with someone who has OCD requires significant compromise, which, as a result, further strains already existing relationships.
There’s plenty of room to build up frustration having an OCD patient around. This happens especially easily with immediate family members whose daily life involves interacting with the patient. This could lead to poor family function and potentially serious complications with family members’ mental health.
On the other hand, OCD has cost the global economy an estimated 6.2 billion US dollars in losses a year. This number might seem exaggerated, but it is reasonable compared to other mental-health-caused losses and considering the fact that mental health problems accounts for one of the largest single contributor of economic health burden in the world, with an estimated global cost of $2.5 trillion US dollars – greater than cardiovascular disease, chronic respiratory disease, cancer, or diabetes.
So how could we help to reduce further negative effects of OCD on socially and economically? One of the easiest ways to encourage people with OCD to take a specific treatment. Studies have shown that specific treatments, such as serotonin reuptake inhibitors and behavior therapy showed greater symptom improvement, and significantly reduced the total cost incurred by OCD patients.
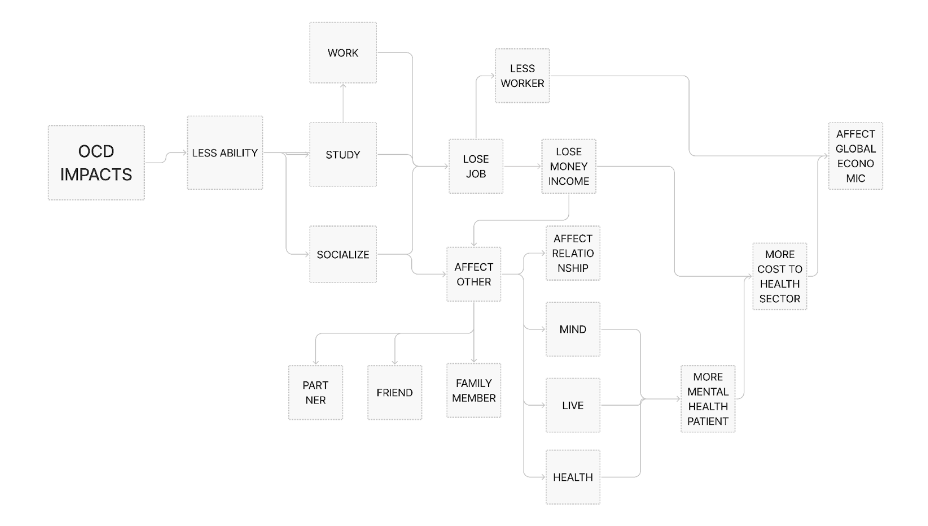
Diagram 1. Impacts of OCD
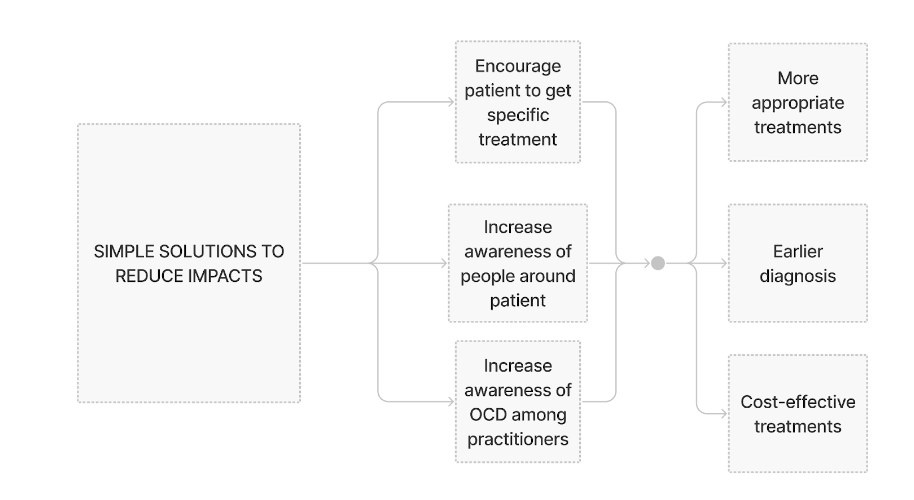
Diagram 2. Solutions to Reduce Impacts
Treatments
Pharmacotherapy
Clomipramine, a potent Serotonin Reuptake Inhibitor (SRIs), was the first to receive FDA approval for OCD treatment. However, due to its adverse side effects, it is not generally well tolerated by patients with OCD, leading to high discontinuation of medication — up to 90% in some studies. Thus Selective Serotonin Reuptake Inhibitors (SSRIs) are preferred as the first-line treatment for OCD.
Psychotherapy
Cognitive Behavioral Therapy (CBT) has become one of the main lines of treatment for OCD.The efficacy of CBT is equivalent or superior to Pharmacotherapy’s SSRI medications or even combined therapy in some studies; however, 50-60% of patients are resistant to the treatment, and relapse rates on discontinuation are relatively high due to a lack of motivation and engagement.
Surgical and Neuromodulatory Treatments
Electroconvulsive Therapy (ECT)
Electroconvulsive therapy (ECT), induces seizures under narcosis electrically, is regularly used to treat major depression. However, the literature on ECT in obsessive-compulsive disorder (OCD) is sparse, and most clinicians do not perceive ECT as a valid treatment option for OCD. Case studies suggest ECT may be effective only for the comorbid affective or psychotic disorders of OCD cases.
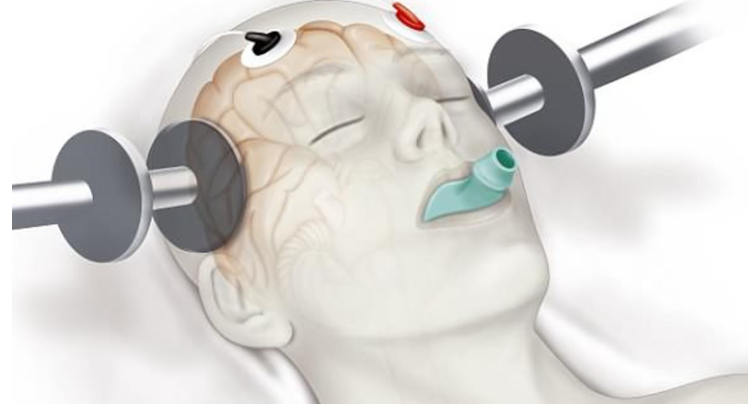
Figure 1. ECT (dailymail.co.uk/)
Transcranial Magnetic Stimulation (TMS)
TMS modulates local neural activity by inducing a depolarizing magnetic field pulse. The device stimulates the human cortex directly by a contactless and non-invasive method. It uses a strong pulse of electrical current, which is sent through a coil and induces a magnetic field pulse in the area under the coil. This pulse has the capacity to depolarize superficial local neurons (Zohar, 2012, p.77). Local induction of a depolarizing magnetic field pulse decreases obsessive-compulsive symptoms by normalizing hypermetabolism in orbitofrontal-striatal circuits. The technique is non-invasive and has zero or very mild side effects, of which headache is the most common. Sadly, the efficacy of this method is still unclear due to the lack of studies with comparable stimulation or treatment parameters and reliable designs.
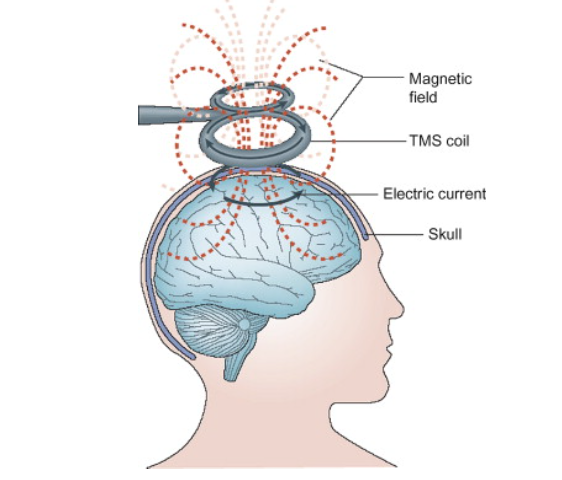
Figure 2. TMS (sciencedirect.com )
Deep Brain Stimulation (DBS)
Since OCD has been associated with hyperactivity of the cortico-striato-thalamocortical (CSTC) network, electrical stimulation is assumed to be effective as it induces a resetting of network oscillatory patterns across the CSTC network. Overall, DBS in OCD may decrease 40–60% of symptoms in at least half of patients. DBS has the potential to become the preferential treatment for a specific group of seriously ill, therapy-refractory OCD patients due to the low risk of the operation, the reversible nature of the technique, and the possibility to optimize treatment postoperatively (Zohar, 2012, p.94).
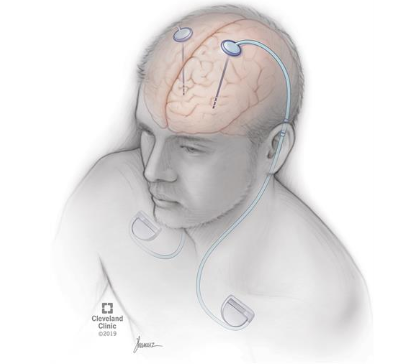
Figure 3. DBS (cleavelandclinc.org)
Surgical Lesioning
In the case of severe treatment-refractory OCD, an OCD patient might be a candidate for neurosurgical treatment. Procedures were undertaken to disconnect brain targets in the emotional system physically. The most common lesioning treatments for treatment-refractory OCD are anterior capsulotomy and anterior cingulotomy, performed using traditional surgical techniques or stereotactic radiosurgery. Overall, lesioning procedures offer therapeutic benefits to 30–60% of patients with treatment-refractory OCD.
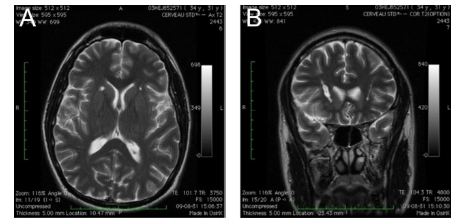
Figure 4. Anterior Capsulotomy (jnnp.bmj.com)
References
Bream, V., Challacombe, F., Palmer, A., & Salkovskis, P. (2017). Cognitive Behaviour Therapy for Obsessive-compulsive Disorder (1st ed.). Oxford University Press.
Stein, D., & Hollander, E. (2002). Textbook of Anxiety Disorders. American Psychiatric Pub.
Schatzberg, A. F., & Nemeroff, C. B. (2017). The American Psychiatric Association Publishing Textbook of Psychopharmacology. Van Haren Publishing.
https://psycnet.apa.org/doi/10.1001/archpsyc.1980.01780240087010
Zohar, J. (Ed.). (2012). Obsessive compulsive disorder: Current science and clinical practice. Wiley-Blackwell. https://doi.org/10.1002/9781119941125
https://thejns.org/view/journals/j-neurosurg/124/1/article-p077.xml
https://www.psychiatry.org/patients-families/ocd/what-is-obsessive-compulsive-disorder
Mathes BM, Morabito DM, Schmidt NB. Epidemiological and Clinical Gender Differences in OCD. Curr Psychiatry Rep. 2019 Apr 23;21(5):36. doi: 10.1007/s11920-019-1015-2. PMID: 31016410.
https://www.psychiatry.org/patients-families/ocd/what-is-obsessive-compulsive-disorder
https://www.verywellmind.com/ocd-risk-factors-2510484 (PANDAS)
https://www.mayoclinic.org/diseases-conditions/obsessive-compulsive-disorder/symptoms-causes/syc-20354432 OCD risk factors (Born with, controlled/uncontrolled situations, Modifiable)
https://jurnal.ugm.ac.id/buletinpsikologi/article/view/32807
https://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.681.2122&rep=rep1&type=pdf
https://www.ocduk.org/ocd/social-and-economic-impact-of-ocd/
About OCD. International OCD Foundation website. Available at: https://iocdf.org/about-ocd. Accessed January 13, 2020.
Moretti G, Pasquini M, et al. What every psychiatrist should know about PANDAS: a review. Clin Pract Epidemol Ment Health. 2008 ; 4:13.
Obsessive-Compulsive Disorder (OCD). EBSCO DynaMed website. Available at : https://www.dynamed.com/condition/obsessive-compulsive-disorder-ocd. Accessed January 13, 2020.
Obsessive-compulsive disorder (OCD). National Institute of Mental Health website. Available at : https://www.nimh.nih.gov/health/topics/obsessive-compulsive-disorder-ocd/index.shtml. Accessed January 13, 2020.
Comments